Conditions We Treat
motion-preserving, fusion-free spine care
Motion-Preserving, Fusion-Free Spine Care
Spine pain can affect everything; how you sleep, work, move, and show up for your life. At Spine Motion Specialists, we help patients understand the why behind their symptoms and explore motion-preserving, fusion-free spine care options that prioritize mobility, function, and long-term quality of life.
Led by Dr. Scott Hodges, our practice focuses on identifying the true pain generator (disc, nerve, joint, alignment, or stenosis-related compression) and building an individualized plan starting with conservative care when appropriate and escalating thoughtfully when needed.
Common Reasons Patients Seek a Spine Specialist Include:
Chronic neck pain or low back pain
Radiating arm pain or leg pain
(Pinched Nerve / Radiculopathy / Sciatica)
Pain with walking/standing
(possible stenosis)
Loss of motion, stiffness, or instability

Degenerative Disc Disease (DDD)
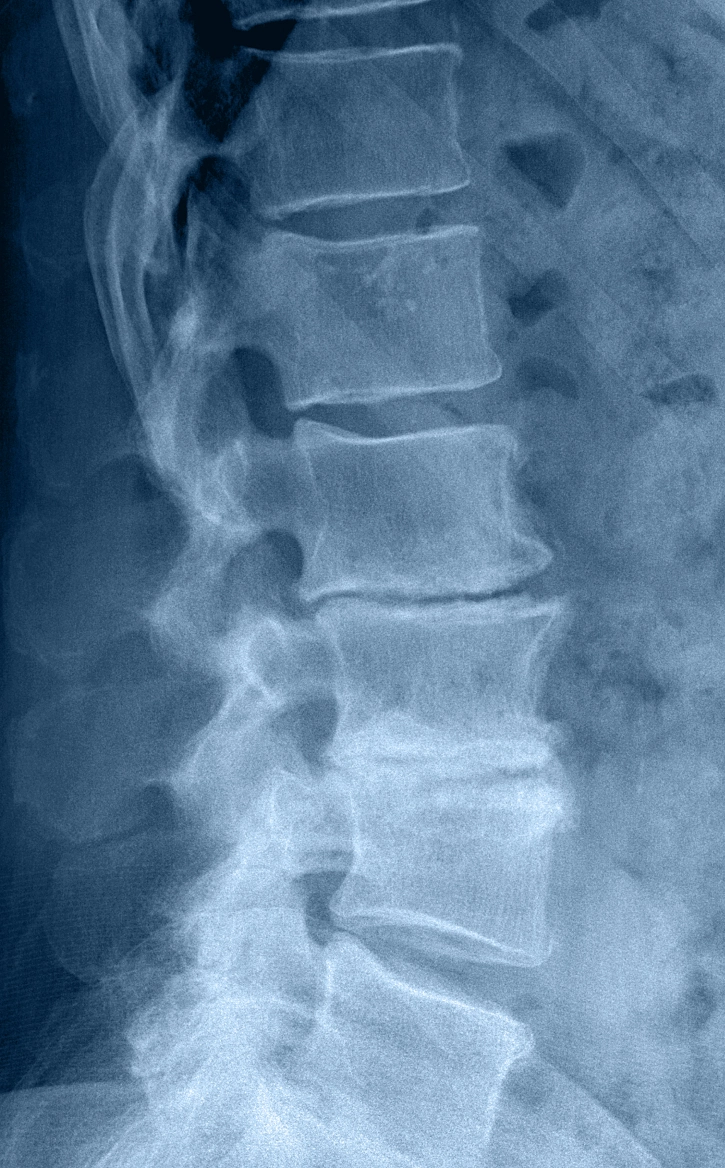
What is it?
Occurs when spinal discs lose hydration and elasticity over time, reducing their ability to absorb impact and support smooth motion.
How it Happens?
Most commonly age-related disc changes, sometimes accelerated by repetitive strain, posture, smoking, genetics, or prior injury.
Symptoms
Chronic neck or low back pain, stiffness, and sometimes radiating pain into arms or legs—often worse with sitting, bending, or twisting.

Herniated Disc
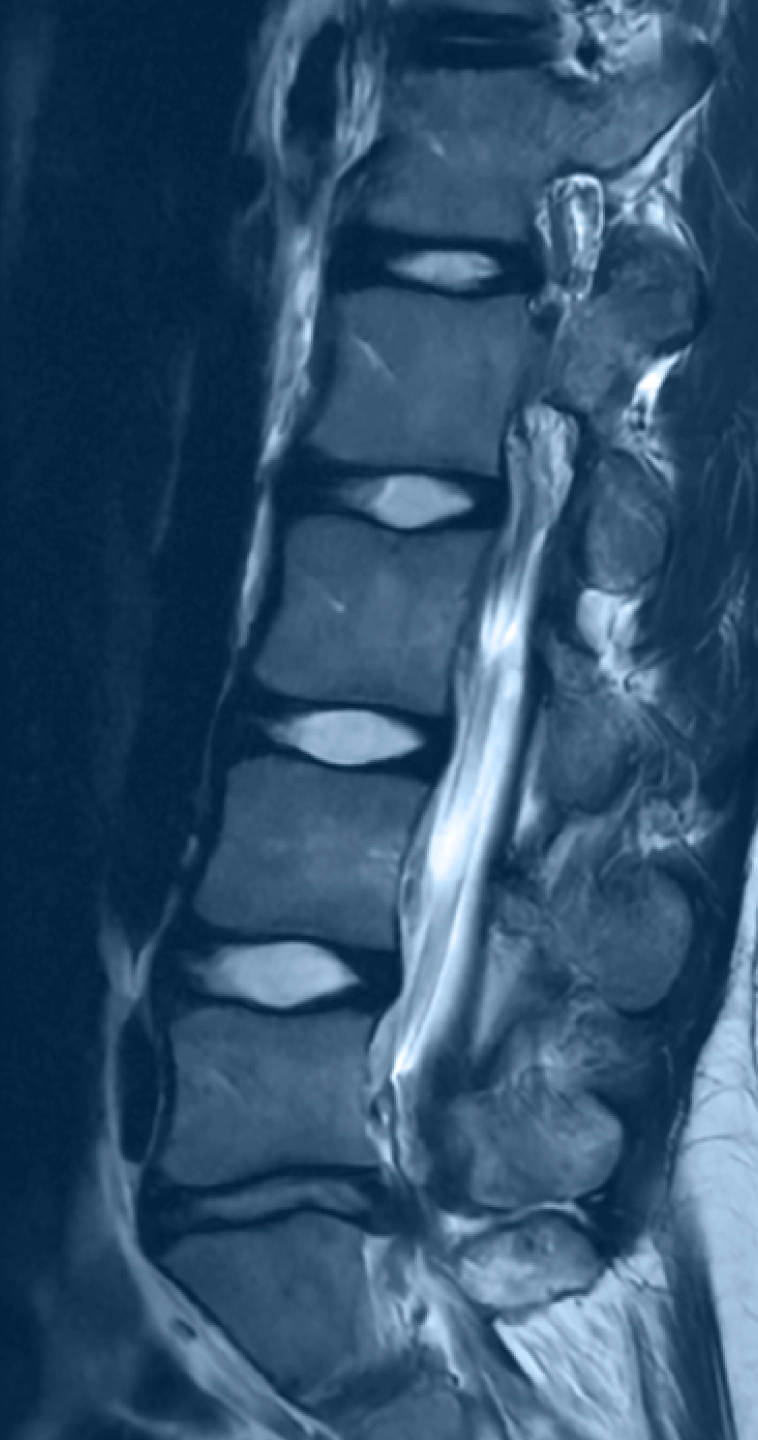
What is it?
A herniated disc occurs when the disc’s soft center pushes through a tear in the outer layer and can press on nearby nerves.
How it Happens?
Often from gradual disc degeneration; sometimes triggered by lifting, twisting, or trauma.
Symptoms
Sharp or radiating pain, numbness, tingling, or weakness in the arm or leg—often worse with sitting, coughing, or bending.

Spinal Stenosis
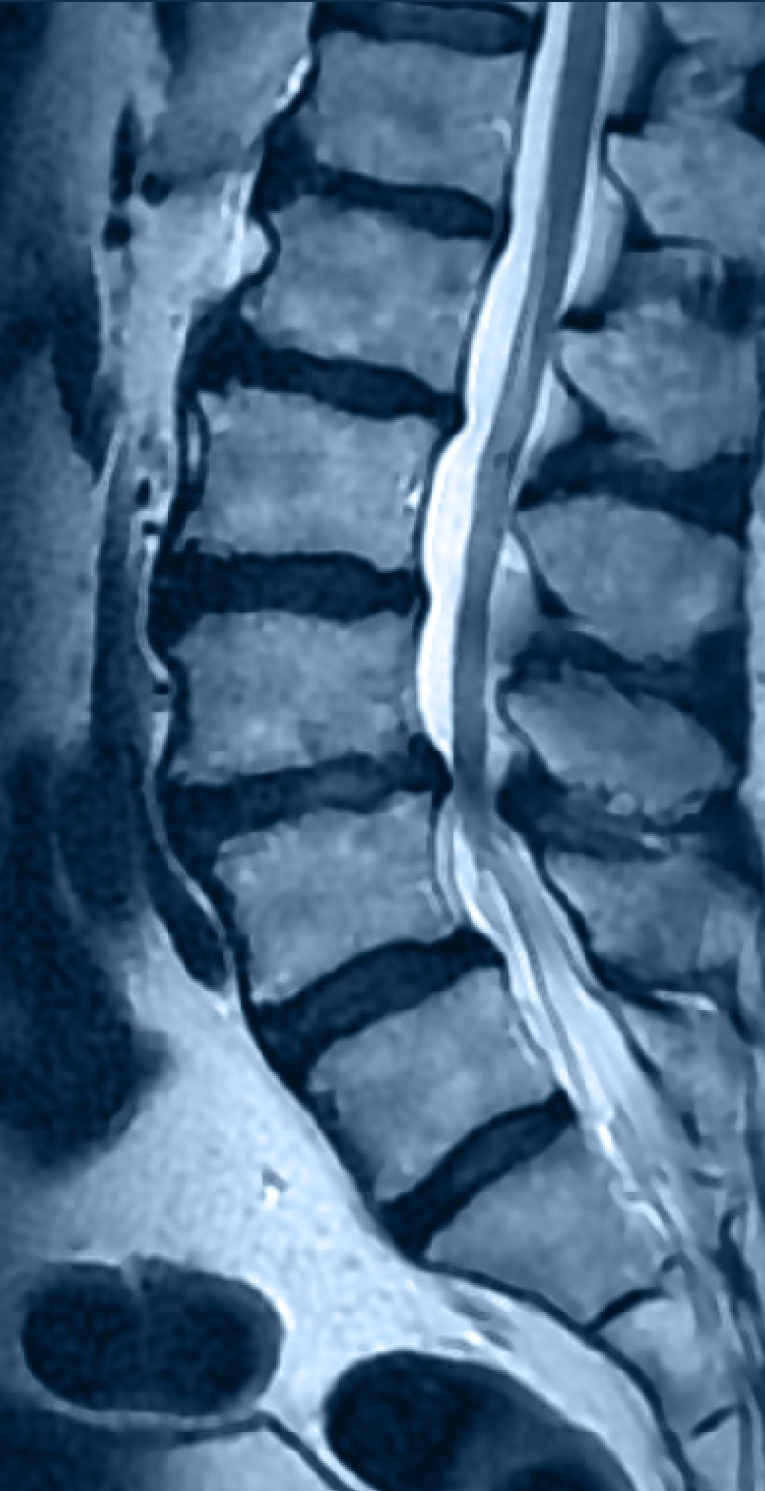
What is it?
Spinal stenosis is narrowing inside the spine that compresses nerves or the spinal cord (lumbar or cervical).
How it Happens?
Age-related changes like disc shrinkage, thickened ligaments, and bone spurs; sometimes arthritis or prior injury.
Symptoms
Back/neck pain, numbness/tingling/weakness, and leg heaviness or cramping with walking/standing (neurogenic claudication).

Spondylolisthesis
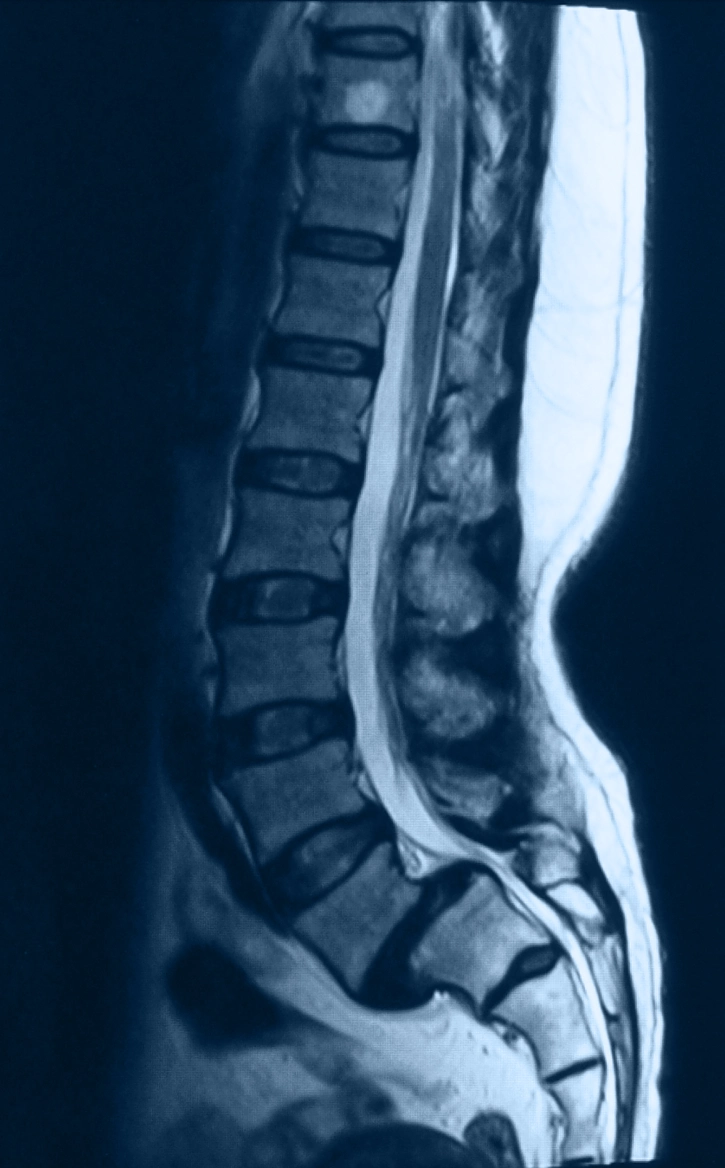
What is it?
Spondylolisthesis occurs when one vertebra slips forward over another, which can create instability and nerve compression.
How it Happens?
Degenerative changes in adults; stress fractures, congenital factors, or trauma in younger patients.
Symptoms
Low back pain, stiffness, tightness, and possible radiating leg symptoms; sometimes difficulty walking or reduced flexibility.

Sciatica
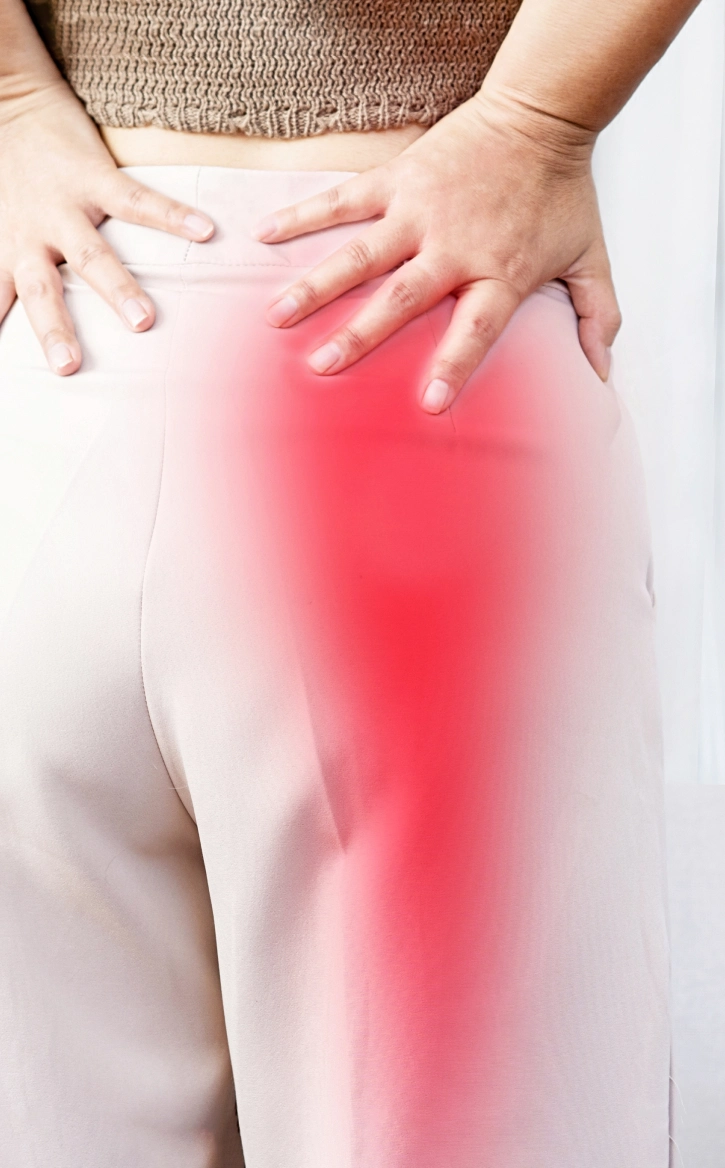
What is it?
Sciatica is radiating pain along the sciatic nerve—typically from low back through the buttock and down the leg—caused by nerve irritation or compression.
How it Happens?
Most commonly a herniated disc; also spinal stenosis, bone spurs, or degenerative narrowing.
Symptoms
Sharp, burning, or electric-like leg pain with possible numbness/tingling/weakness that limits daily function.

Kyphosis
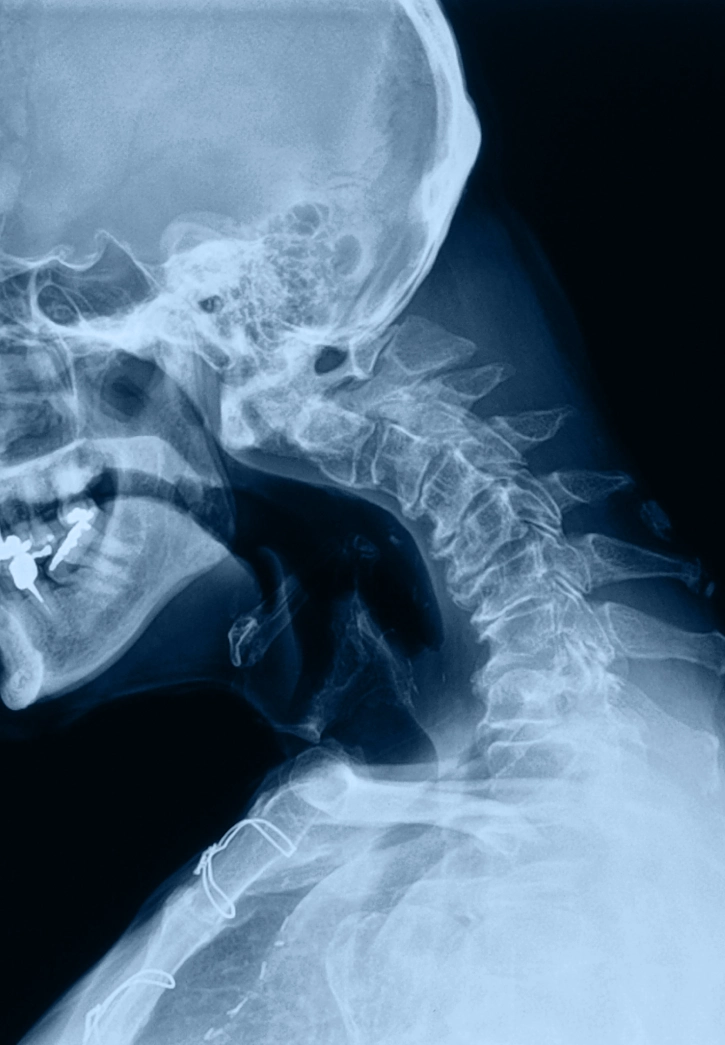
What is it?
Kyphosis is an exaggerated forward curve of the upper back that can create a rounded posture.
How it Happens?
Degeneration or compression fractures in older adults; Scheuermann’s kyphosis in adolescents; sometimes posture-related muscle weakness.
Symptoms
Visible rounding, pain, stiffness, fatigue, and (in severe cases) breathing limitations; may also affect the neck.

Scoliosis
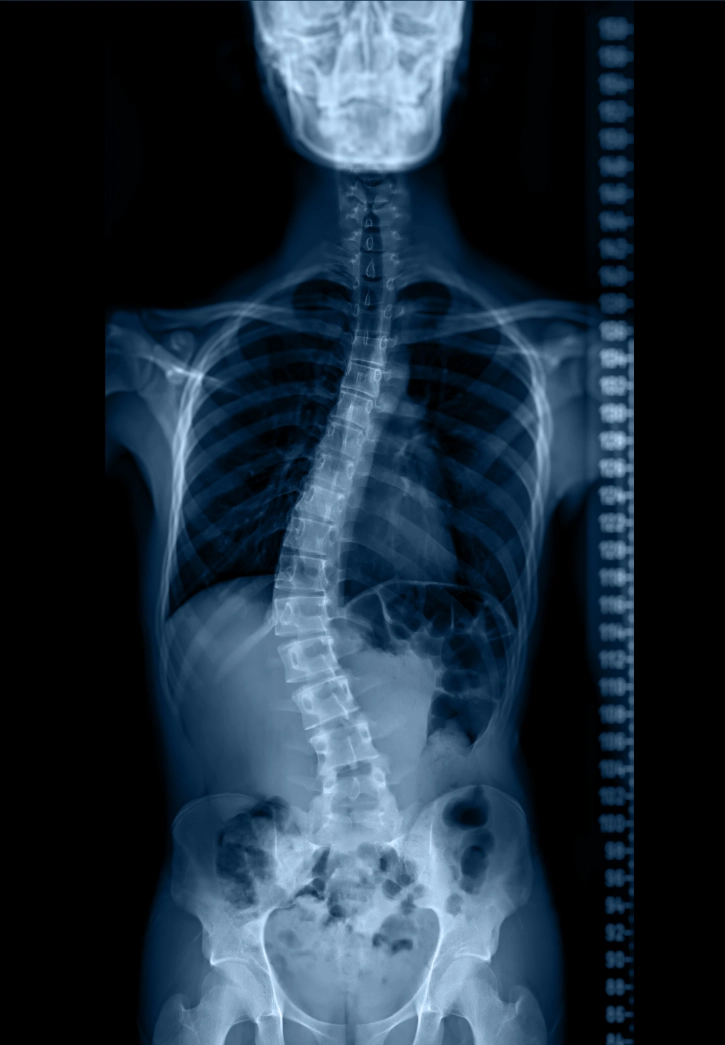
What is it?
Scoliosis is an abnormal sideways curve of the spine, often “S” or “C” shaped.
How it Happens?
Idiopathic (unknown) in many youth; can also be congenital, neuromuscular, or degenerative in adults.
Symptoms
Uneven shoulders/hips, posture changes, back pain, fatigue, and sometimes nerve symptoms if compression occurs.

Facet Arthritis
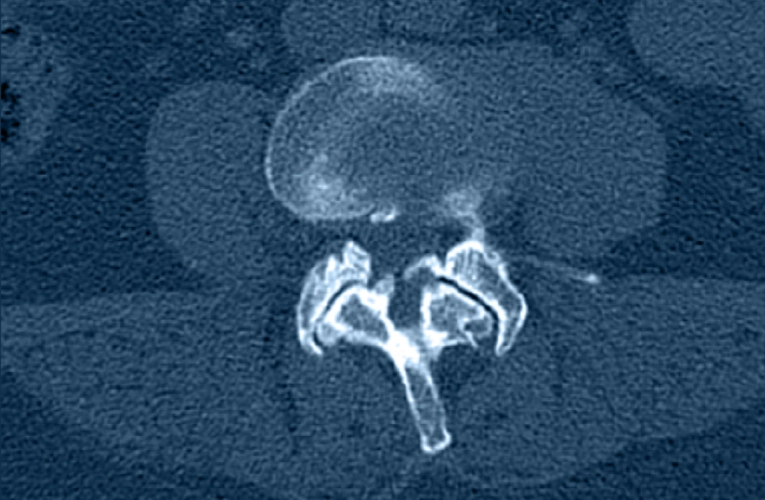
What is it?
Facet arthritis involves wear-and-tear of the small joints in the back of the spine that guide motion and provide stability.
How it Happens?
Osteoarthritis and repetitive stress; can be worsened when discs lose height and load shifts to the facet joints.
Symptoms
Localized neck or low back pain and stiffness—often worse with extension/side-bending and improved by bending forward.

Annular Tear
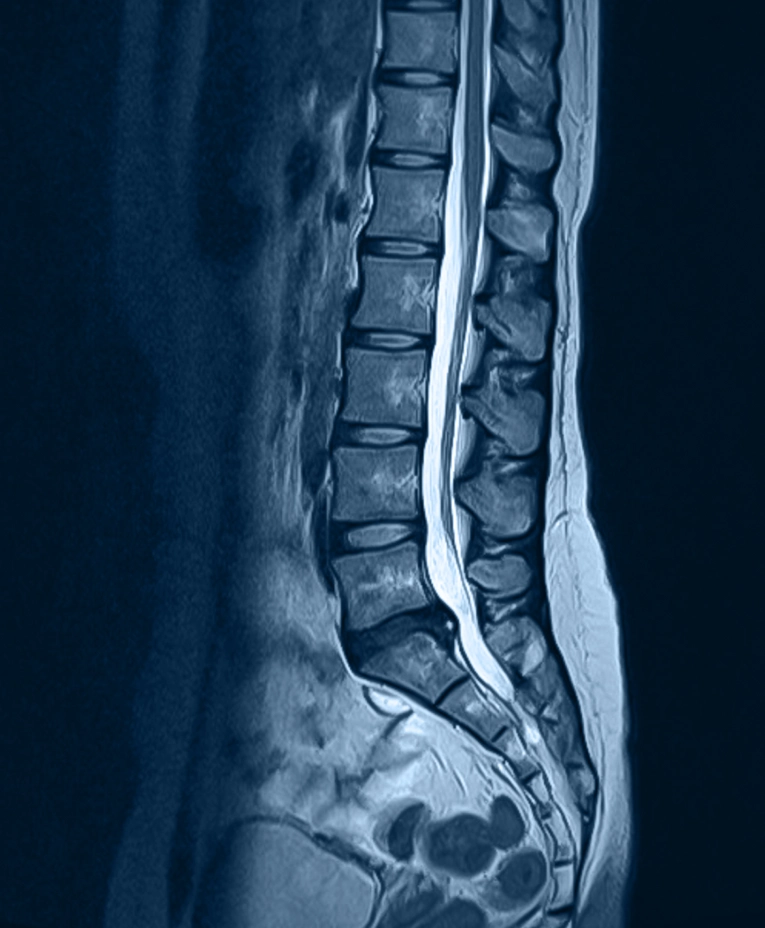
What is it?
An annular tear is a small rip in the tough outer ring of a disc, which can cause inflammation and pain and may increase the risk of future herniation.
How it Happens?
Often from disc dehydration and degeneration; sometimes from lifting injuries, twisting, falls, or accidents.
Symptoms
Local back/neck pain; sometimes radiating symptoms if nearby nerves become irritated.

Radiculopathy

What is it?
Radiculopathy occurs when a spinal nerve root is compressed or inflamed, causing radiating pain, numbness, tingling, or weakness.
How it Happens?
Herniated discs, bone spurs, stenosis, or degenerative changes that narrow nerve exit pathways.
Symptoms
Cervical radiculopathy: neck pain into shoulder/arm/hand
Lumbar radiculopathy: low back pain into buttock/thigh/leg/foot

Failed Back Surgery Syndrome (FBSS)
What is it?
Failed Back Surgery Syndrome (FBSS) describes persistent or recurrent back or leg pain following one or more spine surgeries. Also referred to as chronic postoperative spine pain, FBSS is not a single diagnosis but a complex condition involving unresolved nerve compression, scar tissue formation, mechanical instability, or degeneration after prior surgery.
How it Happens?
Incomplete nerve decompression, epidural scar tissue, recurrent disc herniation, adjacent segment degeneration, biomechanical changes following spinal fusion, or failed spinal instrumentation.
Symptoms
Ongoing low back or neck pain, radiating arm or leg pain, numbness, weakness, burning nerve pain, stiffness, or worsening symptoms months or years after surgery.

Not Sure Which Condition Fits Your Symptoms?
Schedule a consultation and we can help you get clarity and explore motion-preserving treatment options.

Common Questions About Spine Conditions & Care
How do I know which spine condition I have?
Many spine conditions share similar symptoms, which can make things confusing. Back pain, leg pain, stiffness, or numbness can come from discs, nerves, joints, or alignment issues. That’s why we start with a detailed conversation about your story; how your pain began, what makes it better or worse, and how it affects your life. From there, Dr. Hodges performs a focused exam and reviews imaging to identify the true source of your symptoms and guide the right treatment plan.
What symptoms suggest a pinched nerve?
A pinched nerve (radiculopathy) often causes pain that travels, not just local back or neck pain. You may feel sharp, burning, or electric pain down your arm or leg, along with numbness, tingling, or weakness. Sciatica is a common form of lumbar radiculopathy. If your pain radiates or you notice changes in strength or sensation, it’s important to get evaluated so we can protect nerve health and function.
Do all spine conditions require surgery?
Not at all. In fact, most patients improve with non-surgical treatment such as physical therapy, activity modification, medications, or targeted injections. Surgery is only considered when conservative care hasn’t provided relief or when nerve function is at risk. Our philosophy is to start with the least invasive options and move thoughtfully, never rushing to surgery.
What does motion-preserving, fusion-free care mean?
It means your treatment is focused on relieving pain while protecting your ability to move. At Spine Motion Specialists, we do not offer spinal fusion. Instead, Dr. Hodges specializes in solutions that maintain natural spine motion whenever possible; whether that’s through non-surgical care, minimally invasive procedures, or motion-preserving surgery like disc replacement. The goal is to help you feel better without sacrificing long-term mobility or function.
When should I see a spine specialist?
If your pain lasts more than a few weeks, interferes with sleep or daily activities, or keeps you from doing the things you love, it’s worth getting clarity. You should also seek care if you experience radiating pain, numbness, tingling, or weakness. Early evaluation can help prevent symptoms from worsening and open the door to more treatment options.
Can travel patients start with a virtual consultation?
Absolutely. Many of our patients live out of state or internationally and begin with a virtual consult. This allows Dr. Hodges to review your history, imaging, and symptoms, answer your questions, and determine next steps before you travel. We make the process clear, personal, and well-supported from the start.
How is Spine Motion Specialists different from other practices?
We are a concierge, cash-pay practice built around time, access, and individualized care. You work directly with Dr. Hodges from your first visit through recovery. Appointments are unhurried, your questions are always welcome, and your treatment plan is built around you, not a protocol.
What if I’ve been told fusion is my only option?
Many patients come to us after hearing this. In many cases, there are motion-preserving alternatives that may be appropriate. While fusion can be necessary in some situations, our practice is dedicated to exploring options that protect mobility whenever possible. A consultation can help determine what solutions make sense for your specific condition and goals.